What is melanoma?
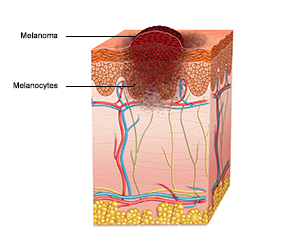 Melanoma is a form of cancer that forms in cells in the skin called melanocytes. The melanocytes make melanin, a pigment that give skin its colour. Common locations for melanoma to start are the neck, face, chest and back (particularly in men) or on the legs (the most common site for women). In 2018, 3,882 Ontarians (2,161 males and 1,721 females) were diagnosed with melanoma and 487 died from the disease.*
Melanoma is a form of cancer that forms in cells in the skin called melanocytes. The melanocytes make melanin, a pigment that give skin its colour. Common locations for melanoma to start are the neck, face, chest and back (particularly in men) or on the legs (the most common site for women). In 2018, 3,882 Ontarians (2,161 males and 1,721 females) were diagnosed with melanoma and 487 died from the disease.*
The skin is the largest organ in the body and skin cancer is the most common cancer in Canada. In addition to melanoma, there are 2 types of non-melanoma skin cancers: squamous cell and basal cell carcinoma.
If discovered early, melanoma is often curable. But melanoma can spread to other parts of the body. For example, melanoma can grow into the deep layers of the skin and enter the lymph nodes. Using the lymph system, the cancer can then travel to other parts of the body (i.e., metastasize). If melanoma spreads to other organs, it can be extremely difficult to treat. It is critical to:
- Make changes to reduce the risk of developing melanoma
- Know your skin so you can recognize unusual or new bumps or growths
Melanoma is one of the most preventable forms of cancer. If discovered early, it may also be very treatable. But wait too long and melanoma cancer can spread throughout the body.
The single most important risk factor for melanoma and non-melanoma skin cancer is exposure to ultraviolet radiation (UVR). By the time sunlight reaches the earth, it consists largely of 2 types of UVR: UVB and UVA. UVB rays are the most damaging to the skin. In Ontario, UVB is more intense in the summer, particularly between 11 a.m. and 3 p.m. UV radiation also increases with altitude and can be intensified by reflective surfaces such as water, snow, ice, concrete or sand. UVR prematurely ages the skin, causes sunburns and may result in genetic mutations that lead to skin cancer.
*The source of data used in the My CancerIQ Melanoma Risk Assessment is based on people who were assigned male or female at birth. Because of this, gender binary language (male, female, man, woman) may sometimes be used. If your gender is different from your sex assigned at birth, My CancerIQ may not assess your risk accurately. Talk to your doctor or nurse practitioner about your risk of developing melanoma.
Risk factors you can change or control
Some of the factors that increase or decrease your risk of melanoma are things you cannot change or control, such as the colour of your skin, your family medical history, or whether or not you have moles. But the single most important risk factor for melanoma is something you can change or modify: your exposure to UVR (ultraviolet radiation).
Exposure to UVR
Compared to people with little sun exposure, those who spend a lot of time in the sun have an increased risk of melanoma. Intense exposure or over-exposure to sunlight may be associated with an even greater risk of melanoma – up to 60% higher.
The amount of skin damage from UVR depends upon:
- The strength of the sun’s rays (time of year, time of day and where you are)
- How long your skin is exposed
- Personal characteristics such as eye and hair colour and how your skin reacts to UVR
- Whether you use protection such as clothing, a hat, shade, sunscreen, and sunglasses
Studies have shown that frequent sunburns -- even if they occurred years ago when you were a child or teenager -- increase the risk of melanoma. You cannot change what happened in the past but you can take action to reduce damaging UVR exposure in the future. Remember – whether it is sunburn or suntan, any change in the colour of the skin is a sign it has been damaged.
Tanning equipment
Tanning equipment, such as tanning beds or lamps, emit the same damaging UVA and UVB rays as the sun. As a result, people who use tanning equipment have at least a 20% increased risk of melanoma. The younger you are when you start using tanning equipment and the more frequently you use it, the greater your risk. The risk is especially high if you used this equipment before age 35.
As well as damaging the skin, damage to the eyes can occur when using tanning equipment.
Moles
Moles (nevi) are clusters or clumps of melanocytes, the cells that produce the pigment melanin. They appear as dark patches, growths or bumps. Some children are born with moles. But in most cases, moles appear as a result of exposure to UVR, typically before age 20. Reducing exposure to UVR, especially early in life, can help to reduce the chances of developing moles.
Most moles are benign, meaning they are not cancerous. Dysplastic nevi are moles that may be larger, have more irregular shapes or have less uniform colour than most moles. Although they can look like melanoma, they are usually benign.
If the DNA (genetic material) of the melanocytes is damaged, a mole can become cancerous. People with many moles, including those with dysplastic nevi, may be at increased risk of melanoma. To catch any changes early, people with moles should be aware of their size, number, colour and appearance and look out for any changes or new moles.
Risk factors you cannot change or control
Skin, eye and hair type
People who do not tan easily when they are in the sun or who have fair-coloured skin are more susceptible to UVR damage. People with naturally blond or red hair or blue, green or hazel eyes often have skin that is more easily damaged.
In the U.S. it has been estimated that the risk of melanoma is 10 times higher for white Americans than African Americans. Although melanoma is somewhat rare among people with very dark skin, they are not immune. Melanoma can occur in people with darker skin and may be harder to detect early. Even if your natural skin colour is dark it is important to protect yourself from UVR.
Immunosuppressive therapy
Immunosuppressive therapy refers to a regimen of drugs to suppress or weaken the body’s immune response. This sort of therapy is often used for long periods of time by people who have had an organ transplant or an auto-immune condition such as inflammatory bowel disease (Crohn’s disease or colitis) or rheumatoid arthritis. Immunosuppressive medications may make it harder for the body’s immune system to get rid of unhealthy or damaged cells and fight cancer.

Family history
There is evidence that people with a first-degree relative, such as a biological parent, sibling or child (i.e., an immediate family member related to you by blood) with a history of melanoma may also have an increased risk of developing this form of cancer. The more first-degree relatives you have with melanoma, the higher your risk. The risk may be due to a combination of genetic factors, such as similar hair, eye or skin colour, and shared behaviours, such as tanning. There are also some rare genetic conditions that can increase the risk of specific types of melanoma.
Personal medical history
People who have had basal cell or squamous cell carcinoma (non-melanoma skin cancer) are at increased risk of developing another type of skin cancer, including melanoma. People who have had melanoma also have a higher risk of developing another melanoma. Although they are usually benign, people with dysplastic nevi (moles) may also be at increased risk of melanoma.
What you can do to protect yourself
There are several things Ontarians can do to protect themselves against melanoma:
- Enjoy the sun safely – check the UV Index and plan to protect yourself
- Avoid tanning equipment
- Know your skin so you can recognize changes or the need for a skin examination
Check the UV Index
Before planning outdoor activities, check the UV (ultraviolet) Index forecast for your region. It is typically part of the weather forecast and is available online, on TV, on the radio or in the newspaper. The UV Index is a measure of the intensity of the sun’s UV rays. In Canada, the scale ranges from 1 to 11 but the UV Index can reach 14 or higher in tropical areas or the southern U.S. The higher the number, the stronger the sun’s rays and the greater the danger of skin damage. When you know you will be outside, consult the UV Index and make a plan to protect yourself.
Learn more about the UV Index at the Government of Canada website.

Practice sun safety
When the UV Index is 3 or more, or when UV rays may be intensified by reflecting off water, snow or ice, it is important to follow the 5 key sun safety strategies:
- Seek shade.
- Slip on protective clothing.
- Slap on a hat.
- Slop on sunscreen.
- Slide on sunglasses.
Learn how to keep the children in your life safe in the sun
- Always protect babies from the sun and limit sun exposure, especially during peak hours (in Ontario 11 a.m. to 3 p.m., March to October).
- Cover your baby in loose clothing and make sure he/she is wearing a hat.
- Use a stroller sunshade to cover your baby.
- On any part of the body that is not shaded or covered with protective clothing, apply a small amount of sunscreen with a sun protection factor (SPF) of 30. Remember to put sunscreen on vulnerable parts such as the ears, nose, back of neck and legs, and tops of the feet. Before using a sunscreen, be sure to test it on a small area to ensure the child is not allergic to it.
More information on sun safety for children is available from
Learn more about sun safety from the Canadian Dermatology Association.
Check with your local Public Health Unit for more sun safety information and tips. To find your nearest Public Health Unit, visit the Ontario Ministry of Health website.
Seek shade
During peak periods when the UV Index is 3 or higher (in Ontario, 11 a.m. to 3 p.m. between March and October) seek shade to reduce your exposure to damaging UV rays. Tall, deciduous trees with dense, wide canopies and low foliage create the most shade and are the best sources of natural sun protection.
Human-made shade structures include gazebos, verandas and awnings. The amount of protection depends upon:
- The type of material the structure is made from (e.g., sun cannot penetrate wood but may penetrate certain fabrics)
- Whether the structure blocks sun from the sides as well as from overhead. This is particularly important if you are near water or on a surface such as sand or concrete that reflects sunlight.
If there are no natural or human-made sources of shade, you can bring your own umbrella, beach cabana, tent or other portable structure. The amount of protection depends on what it is made of and its design. Some umbrellas or cabanas are made out of fabric that is treated to block UV rays. If that is the case, look for information on the ultraviolet protection factor (UPF) of the fabric.
Learn how to make your own shade at the Canadian Cancer Society.
Slip on protective clothing
Appropriate clothes can be better at protecting your skin against the sun than sunscreen. The best protection is provided by long-sleeved shirts and long pants or skirts made from tightly-woven, dark-coloured fabrics. Loosely-woven and light-coloured fabrics are less protective. Some summer clothing is made with fabric that has been treated with chemicals to increase their ultraviolet protection factor (UPF). If buying UPF-treated clothing, look for a UPF rating of 15 or more.
Learn more about sun protective clothing from the Canadian Dermatology Association.
Slap on a hat
A wide-brimmed hat made out of tightly-woven fabric can shade the head, ears and neck. The most protective hats have a brim that is 7.5 centimetres (about 3 inches) wide all around. For children under the age of 10, the brim should be at least 6 centimetres or close to 2 ½ inches. A legionnaire-style hat with back and side flaps also offers good protection. If buying a hat made out of fabric treated to be sun-resistant, look for an UPF (ultraviolet protection factor) of at least 15.
Baseball caps and sun visors are not very helpful because they leave the ears and the back of the neck exposed. If wearing a baseball cap or visor, be sure to use sunscreen on exposed parts of the ears, neck and face.
Learn more about protecting you and your family from the sun from the Canadian Dermatology Association.
Slop on sunscreen
The best defenses against the sun are shade and protective clothing and hats. On any skin that is left exposed to the sun, wear sunscreen. Look for a sunscreen that:
- Is labeled broad-spectrum
- Is water- or sweat-resistant
- Has an SPF (sun protection factor) of at least 30.
Some insect repellents can reduce the effectiveness of sunscreens. If you are using both you may want to use a higher SPF sunscreen and reapply it more often. Apply the sunscreen first, before applying the insect repellent. As a rule, most insect repellents do not need to be re-applied as frequently as sunscreens.
When using sunscreen, remember to:
- Slop it on generously. Most people do not put on enough. Adults need to use at least 35 millilitres (1 ounce), which is about a handful. Literally “slop” it on generously. Do not rub it into the skin.
- Reapply it regularly. If you go into the water, towel yourself, or get sweaty, you need to reapply your sunscreen immediately. Even if you do not get wet or sweaty, you still need to reapply your sunscreen at least every 2 hours. Again, do not skimp – to get full benefits, you need to apply a full amount.
Helpful hints:
- Remember that no sunscreen can protect you 100% from UVR. Always use sunscreen with other strategies, such as wearing protective clothing or seeking shade.
- Check the expiry date on your sunscreen. Old or expired sunscreens are less effective.
- Do not store sunscreen in a place where it is likely to overheat, such as in the car or in direct sunlight. Heat can break down the ingredients and make sunscreens less effective.
- Sunscreens come in different formulations – lotions, gels, sprays, wipes, etc. Read the label for instructions on how to apply the type you are using.
- Before using a sunscreen, test a small amount on your skin, such as the inside of your elbow, once a day for 3 days. If the skin turns red or becomes itchy, you may be allergic to some of its ingredients so try another type or brand.
Learn more about sunscreen at the Canadian Dermatology Association website.
Slide on sunglasses
Melanoma of the eye is rare but can occur when there is damage from UVR. UVR can also increase the risk of other serious eye disorders later in life such as cataracts, damage to the retina, and macular degeneration. Too much sunlight may cause painful temporary inflammation of the eyes similar to “snow blindness.”
To protect your eyes, every time you are outside slide on sunglasses that block 60% to 92% of UVA rays and 95% to 99% of UVB rays. If the label on a pair of sunglasses says “UV absorption 400 nm” or “UV400” it means they protect against 100% of UVA and UVB rays. Wraparound sunglasses protect against sunlight entering from the sides as well as the front.
More information:
- If you are exposed to intense sunlight bouncing off snow or water, choose sunglasses with dark grey or slightly brown or green tints. They will filter out more blue light.
- Polarizing lenses are designed to cut glare from reflection and are good for driving and outdoor activities in the snow or on water.
- Special purpose sunglasses block even more of visible light (up to 97%) and up to 98.5% of UVA and 99% of UVB rays. These sunglasses are good if you are going to be in the sun for long periods of time but they are not recommended for driving.
- There are UV-absorbing soft contact lenses but they only protect the cornea and cannot block the blue portion of visible light. You will still need to wear sunglasses to protect your eyes.
Learn more about sun damage to the eyes at the Canadian Association of Optometrists website.
Bypass the tanning myth
Some people still think a tan is something healthy. In reality, a tan is a sign your skin has been damaged by the sun and is releasing the pigment melanin in an attempt to protect itself. It is a myth that getting a “base tan” protects against sun damage or prevents sunburn. In reality, a tan has a sun protection factor (SPF) of no more than 3 – not enough to protect the skin from damage. Each time you try to tan UVR damages the skin cells, leading to wrinkles, age spots, premature aging and skin cancer. There is no such thing as a safe tan.
If you still want the tanned look, self-tanners and bronzers may be a healthier alternative.
Learn about sunless tanning products at the Canadian Cancer Society website.
Avoid tanning beds or sunlamps
Because UVR is a carcinogen (cancer-causing agent), it is illegal in Ontario for tanning salons to serve people under the age of 18. Several studies have shown that using indoor tanning devices even once may increase the risk of melanoma by at least 15%. The more frequently tanning equipment is used, the greater the risk of melanoma. The risk of melanoma also rises when the use of tanning beds starts earlier in life, such as before age 35.
Learn more about the dangers of indoor tanning at the Canadian Dermatology Association website.
Know your skin
It is important to know your skin. Examine your skin regularly to look for warning signs such as:
- A change in the shape, colour, size or surface of a birthmark or mole
- A sore that does not heal
- Any patch of skin that bleeds, oozes, swells, itches or becomes red and bumpy
It is a good idea to periodically check moles so you are aware if they start to change. Use the ABCDE system to help you identify possible signs of melanoma.
- Asymmetry: if you were to draw a line through the mole or growth, the two halves would not match (e.g., one half is a different shape or colour than the other half)
- Borders: the edges are irregular, scalloped or notched
- Colour: there may be a mixture of different colours, such as shades of tan, brown or black, or sometimes even white, red or blue within the same mole, sore, lump or growth
- Diameter: keep an eye out for any spot that grows larger, particularly if it is bigger than 6 millimetres (about ¼ inch) in diameter
- Evolving: the border, colour, elevation, shape or diameter changes or there is a new symptom such as bleeding, itching or crusting.
If you notice any change or new development, consult your doctor or nurse practitioner.
Learn about the ABCDE rule to help you detect melanoma early at the Canadian Dermatology Association website.
Know about photosensitivity
Some medications or products can make the skin more sensitive to the sun (photosensitivity). When starting a new prescription or over-the-counter medication or herbal remedy, read the product information and talk with your pharmacist. Ask if this product has been reported to increase sun sensitivity. If it does, you should be careful to protect yourself whenever you are in the sun.
Transplant patients have special sun protection needs. You can learn more at the University Health Network: Life after transplant website.


